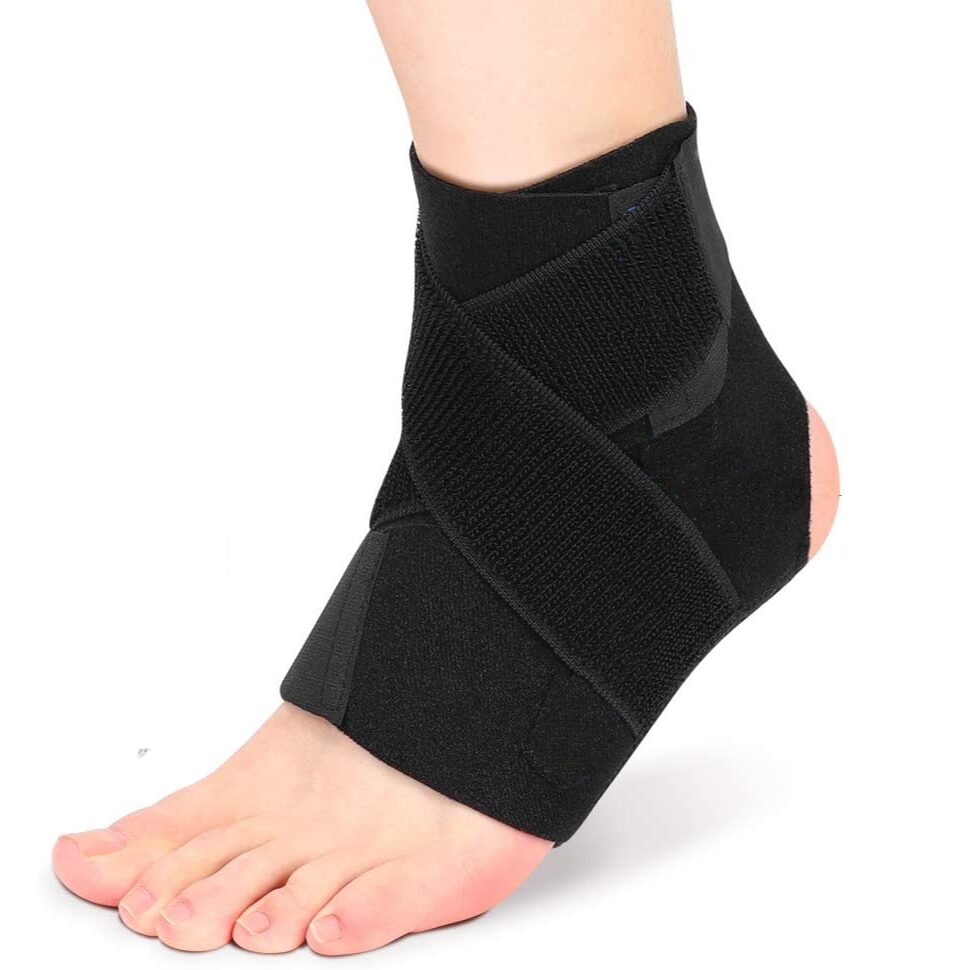
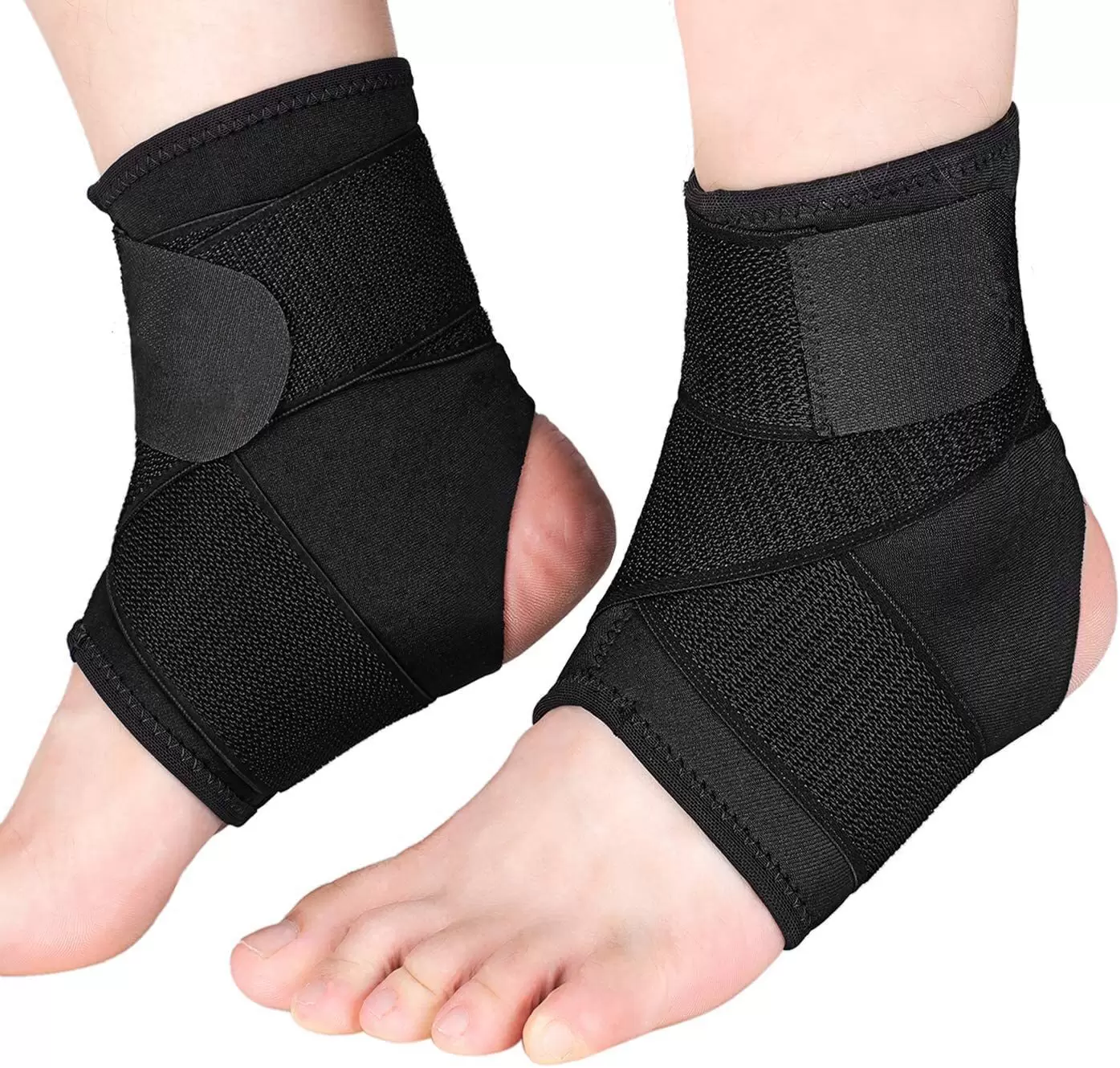
FootReviver™ Plantar Fasciitis Night Splint
$10.79
$15.75
If the first steps out of bed send a sharp stab of pain through your heel, you are not alone. This pattern is very common in plantar fasciitis (often called plantar heel pain) and related heel problems.The pain often feels as if the heel is being jabbed or bruised from the inside with those first few steps, then eases enough to get on with things, only to flare again when standing after sitting or driving. It is not simply “getting older”, and in many cases it can be improved.A key part of the problem is what the foot and calf are doing when you are off your feet, especially overnight, not just how they behave when walking or standing. When the plantar fascia and calf shorten during rest, the first steps after that rest pull on them more sharply than they can comfortably tolerate.The FootReviver™ Plantar Fasciitis Night Splint is designed with this in mind. It holds the foot and ankle in a gently stretched, supported position while asleep or resting. That means the tissues under the foot and at the back of the ankle are not allowed to fully tighten and then be yanked back to working length with the first steps. The aim is simple: to take the sharp edge off those first few steps after sleep and sitting.Used regularly, alongside sensible daytime measures such as suitable footwear, simple stretches and strengthening, this splint offers a practical way to ease first‑step heel pain and make mornings easier to face.This page looks at:The pattern of pain many people recogniseWhat is happening inside the foot and calfHow the FootReviver™ night splint and other simple steps can change thatWho this type of splint is and is not suitable forIf this sounds like your pattern of pain, reading from top to bottom gives the full picture. If you mainly want to check suitability, you can also look at the section “Who This Night Splint Is and Is Not Suitable For” further down.The Problem: Morning Heel Pain and “First‑Step” StiffnessFor many people with plantar fasciitis, the worst pain is not in the middle of the day when busy. It is when trying to get going again after a spell of rest. Typical situations include:Getting out of bed in the morningStanding up from a chair after sitting for a whileStepping out of the car after a driveThe pain is usually under the heel, often slightly towards the inner side, and may run into the arch. It can feel sharp, stabbing, or like stepping on a stone. Many people find themselves holding on to furniture or moving very cautiously for the first few steps, then hobbling to the bathroom until things “warm up” a little. After walking for a few minutes, the pain often settles to a duller ache. Later, after another period of sitting or lying down, the same thing happens again.Even in the short term this affects how the day feels. Those first few minutes can colour the whole start of the morning and make simple things like getting to the bathroom or downstairs feel like a chore.If the pattern carries on, people often begin to:Change the way they walk to avoid loading the sore areaCut back on walking, sport, or family activitiesThese changes are natural short‑term coping strategies, but if they go on for long, they can quietly start to affect how the whole leg loads. That is one reason it is better to tackle the problem than just work around it.This “first‑step” pattern is very common in plantar fasciitis, although other conditions can sometimes cause similar symptoms. To change it, it helps to know what the plantar fascia actually does and what happens to it when you are off your feet.Why Plantar Fasciitis Hurts Most After RestThis section looks at what the plantar fascia does, how it becomes sore, and why those first steps after rest hurt so much.What the Plantar Fascia DoesAcross the bottom of each foot is a thick band of tissue called the plantar fascia. It runs from the heel bone to the base of the toes. Its main jobs are to:Help support the arch of the footShare some of the force every time weight goes through the footStore and release elastic energy with each step, helping the foot work like a springBecause it is involved in almost every step, the plantar fascia deals with repeated strain throughout the day.How It Becomes Irritated and SensitivePlantar fasciitis develops when this tissue is repeatedly overloaded. By overload, this simply means asking it to cope with more strain, more often, or with less recovery than it can handle. It is not always a single injury; more often it is many small strains building up faster than the tissue can recover.Small areas, usually close to where the fascia joins the heel bone, start to show tiny amounts of damage and irritation. When the problem has been present for a long time, the tissue in this area can become more worn and less able to cope, not just inflamed. Ordinary loads that were once fine can then become painful.Common contributors include:Repetitive impact, such as running, jumping, or brisk walking on hard groundLong spells standing or walking at work, especially on concrete or tiles, which give very little natural cushioningFoot mechanics that increase strain on the fascia, such as the foot rolling inwards a lot (overpronation) or having high, rigid archesTight calf muscles and a stiff Achilles tendon, giving less “give” in the back of the lower legChanges in bodyweight or activity level that add more load before the tissues have adaptedAge‑related changes that make soft tissues a little less tolerant of repeated strainIn these situations, more force keeps going through the same small area near the heel, or the tissue has less time to recover between spells on your feet. Over time, a sore, sensitive patch develops that is easily stirred up.Why Mornings and First Steps Feel So BrutalThe familiar “first‑step” pain usually follows a clear sequence:During the day, every step loads the plantar fascia, especially near the heel. When this area is already irritated, that repeated loading keeps it sore.When lying down or sitting for longer periods, the foot is not carrying weight. The plantar fascia and the muscles and tendon at the back of the lower leg (the calf and Achilles tendon) naturally shorten a little in this relaxed position.Most people sleep with their feet relaxed and the toes pointing slightly down. For someone with plantar fasciitis, this lets the fascia and calf shorten further and stiffen in that shortened state overnight.When standing up after sleep or a long sit, full bodyweight suddenly passes through this shortened, sensitised tissue. The fascia is pulled quickly back towards its working length, and that sudden pull through a sore area causes the sharp heel pain felt with the first steps.As walking continues for a few minutes, the fascia and calf warm and lengthen and the pain often eases. The problem is that this cycle repeats after every longer rest. That sore patch is being pulled and re‑pulled. It can feel like the heel is being “re‑injured” with each first step, even though nothing new has happened overnight.That is why, even after a full night’s rest, the first few steps can feel like the worst part of the day. This sudden pull on shortened, sore tissue is exactly the part a night splint is designed to change.Why Foot Position During Sleep MattersThe plantar fascia and calf shorten when relaxed, especially overnight, and this drives much of the first‑step pain. This section looks at the positions the feet tend to fall into during sleep and how a night splint can counter them.Common Foot Positions in BedMost people do not think about what their feet are doing in bed. A few patterns crop up again and again:Feet lying flat but relaxed so the toes point down a little when on the backFeet hanging over the end of the mattress so the toes drop further downOne leg hooked over the other, twisting the ankle inwards or outwardsAnkles rolling inwards towards each other or outwards away from each other, especially when lying on the sideMost of these positions either increase the toes‑down posture that tightens the fascia and calf, or twist the ankle so tissues around the ankle are pulled unevenly for long periods.How These Positions Affect a Sore HeelWhen the plantar fascia is already sore near the heel:Toes‑down positions allow it to shorten fully and stiffen in that shortened stateThe calf muscles and Achilles tendon do the same, so there is less slack when first movingTwisted or rolled ankle positions put extra stretch on one side of the foot and ankle, pulling on already sensitive tissuesAll of this makes the natural shortening described above worse. By the time the alarm goes off, the fascia and calf are often shorter and stiffer than they were at the start of the night, particularly in people who already have heel or Achilles problems.So if you wake up every morning feeling as if your heel or Achilles has stiffened up again, the way your foot has been sitting overnight is likely to be a big part of the reason.What a Night Splint Is Designed to ChangeA night splint is worn while sleeping or resting and is designed to:Hold the ankle close to a right angleKeep the front of the foot slightly lifted towards the shin, so the toes do not drop downLimit how far the ankle can roll inwards or outwardsIn this position, the plantar fascia and calf–Achilles unit are kept in a gentle, steady stretch instead of being allowed to shorten right down. When standing up again, the tissues start from a better length, so the first stretch is less of a jolt. Over time, this can reduce how strong morning and “after rest” pain feels and give the sore area more chance to settle.That is why what your feet do at night matters just as much as what they do in the day.The same mechanical issue shows up in slightly different ways depending on how someone spends their day. The next section looks at a few common situations where this is particularly obvious.Who Tends to Struggle Most with This PatternThe same basic problem — an irritated plantar fascia and tight calf that shorten at rest, then are pulled sharply when standing — shows up in slightly different ways depending on how someone spends their day. The examples below are not the only situations, but they are common ones.Active People Who Run or Exercise RegularlyPeople who run, go to fitness classes, or play sports such as football or tennis ask a lot of the tissues around the heel. Typical features include:Tight calf muscles from frequent trainingSudden increases in how far, how fast, or how often they exerciseIntroducing hilly routes or tougher sessions without enough build‑upTraining on hard pavements or pitch surfaces that have little giveIn this setting, the plantar fascia and Achilles tendon are loaded heavily, day after day. There is often limited recovery time between sessions, especially if training is frequent.The result is often:A sore heel and stiff calf, particularly the morning after a harder sessionPain when first getting up or going downstairsA pattern of rest, slight improvement, and flare‑up when trying to return to activityHeavy use in the day and extra tightening overnight mean the fascia and calf get pulled sharply every time movement starts again. In this group, the same basic problem is there: sore tissue that tightens when you rest and is then shocked when you stand.People on Their Feet for Long Hours at WorkThose working in retail, hospitality, healthcare, teaching, manufacturing, or warehouses often spend many hours on their feet, often on hard floors. Concrete, tiles and similar surfaces do not absorb much impact, so more force passes straight through the heel with each step.Common features include:Minimal chance to sit down during a shiftFootwear chosen for uniform or safety rules rather than comfort or supportSeveral long days in a row with little time for full recoveryBy the end of a shift, the plantar fascia and calf are often sore and tired. Overnight, these tissues then shorten. The pattern can become:Hobbling out of bed on painful heelsStruggling through the first part of early or long shiftsPain when standing from short breaks, such as lunch or a quick sit‑downHere too, the same pattern is present: heavily used tissue that tightens at rest and is then pulled abruptly when standing.Mid‑Life Changes in Weight or ActivityAround mid‑life, small changes in weight, activity pattern, and old injuries can add up. Common examples are:A few extra kilograms increasing load through the feetLess regular movement, so muscles and tendons are less conditionedLong‑standing issues with ankles, knees, or hips that change how the feet are loadedIn this group, plantar fasciitis often develops slowly:Occasional soreness after busier daysMild heel pain in the morning that used to fade quicklyGradually more frequent and more intense morning painHere, the fascia is dealing with more work on tissues that recover more slowly. Each time rest allows the fascia and calf to shorten fully, the next “restart” pulls on them again. The same basic issue is there: sore tissue that tightens when you are off your feet, then is jolted when you stand.Long‑Standing Heel Pain Put Down to “Wear and Tear”Many people have lived with heel pain for months or years without a clear label. Often they have:Sharp pain under the heel when first standing that eases but never fully disappearsAches after driving, desk work, or evenings on the sofaA tendency to avoid longer walks or certain activitiesWithout a name for it, this pain is often blamed on “wear and tear” or age. People may gradually change the way they stand and walk to avoid loading the sore area, which can increase strain on other parts of the foot and leg.In many of these cases, the same pattern is there: a sore patch in the fascia near the heel that shortens when resting and is then pulled sharply when standing. Recognising this makes it easier to see how changing what happens when off the feet — for example, with a night splint — may help, alongside addressing daytime loads.In all of these situations, the same problem is there: sore tissue that tightens when you rest and is then shocked when you stand. The FootReviver™ night splint is built to change that part of the pattern while you sleep.How the FootReviver™ Plantar Fasciitis Night Splint WorksThe FootReviver™ night splint is built around one aim: to reduce how sharply sore tissues are pulled after rest. It is designed specifically around the classic plantar fasciitis and first‑step pattern described above.Holding the Ankle and Foot in a Helpful PositionWhen fitted, the FootReviver™ splint:Sits along the front of the lower leg and the top of the footHolds the ankle close to a right angleGently lifts the toes towards the shinThis puts a light, steady stretch through both:The plantar fascia under the footThe calf muscles and the Achilles tendon at the back of the ankleThe aim is a gentle, steady pull — enough to lengthen a little, not enough to cause strong pain or cramp.Because the fascia and calf are held nearer to their daytime length:They do not have the chance to fully shorten and stiffen overnightThe change in length needed when standing is smallerLess sudden tension is placed through the sore area near the heelIn other words, the splint reduces how sharply those tissues are pulled when weight is first put through the foot after sleep or a longer sit. This is the bit the night splint is designed to change.Preventing Unhelpful Twists and Droops in BedWithout any support, feet often end up:Hanging off the end of the mattress with toes pointing downCrossing over one another, twisting the ankle inwards or outwardsRolling inwards or outwards when lying on the sideFor someone with plantar fasciitis, Achilles problems, or ankle weakness, these positions can keep tugging on already irritated tissues.The structure and straps of the FootReviver™ splint are set up to:Stop the foot dropping heavily into a toes‑down positionLimit how far the ankle can roll inwards or outwardsKeep the heel, arch, and lower leg in a more neutral lineFewer extreme positions in the night mean fewer repeated pulls and twists on sore tissues. That gives them a calmer period in which to settle, rather than being irritated each time sleep posture changes.What This Means for Your First StepsIf the fascia and calf are not allowed to shorten completely overnight, they are closer to their working length by morning. That usually means:The first steps after getting up pull on them less abruptlyThe jolt of pain with those first few steps is less severeWalking becomes more comfortable more quicklyStanding after sitting or driving is not such a shock to the heelWith regular use, many people notice that they do not have to hobble for as long first thing, and that standing after rest later in the day is easier. These changes come from the same basic effect explained earlier: the tissues are being held at a better length between bouts of activity, so each restart is less stressful on the sore area. In practical terms, this is what takes the sharp edge off those first few steps after sleep and sitting.Rather than just taking the edge off pain in the short term, the splint targets one of the main mechanical triggers — how sharply sore tissues are pulled after rest — so it works with, not against, longer‑term recovery.Unlike some very rigid night splints with a fixed angle, FootReviver™ is designed to let you start gently and build towards the stretch and support your tissues can tolerate.Design Features and Why They MatterThe previous section focused on what the splint does to the foot and ankle. This section explains how specific design choices help it do that in a way that real people can tolerate and stick with.Adjustable Fit and Stretch LevelFeet and lower legs are all different, and so are people’s pain levels and flexibility. The FootReviver™ splint uses several adjustable straps so that most people can:Secure the foot so it does not slip around insideDecide how much the ankle is held up and how far the toes are liftedSet the level of stretch to something that is effective but still comfortableSomeone with very sensitive, long‑standing pain may need only a slight lift to start with, and then increase the angle a little as things improve. Someone with a stiffer calf may need a different angle than someone whose ankle moves more easily.Being able to adjust these settings helps avoid a common problem seen in clinics with rigid splints that only hold one angle: that fixed position might be fine for one person and too much or too little for another. Fixed‑angle splints can feel fine for some and unbearable for others. FootReviver™ avoids that “all or nothing” problem by letting you make small, progressive changes until you find a stretch your tissues can tolerate.Structured Front Support That Holds Position All NightAlong the front of the splint is a firm panel that runs from the shin to the top of the foot. Straps around the calf, ankle and foot attach to this panel. Together, they:Keep the ankle and toes in the chosen positionReduce the chance of the ankle sagging down as you relax in sleepHelp stop the foot twisting into the positions that make pain worseThis is what allows the splint to hold the foot in the helpful posture described above, even when you move position in the night. The strap layout and front support have been adjusted based on where clinicians regularly see people develop rubbing, pressure and discomfort — across the front of the ankle, the shin, and the top of the foot — particularly in those who sleep with their feet hanging off the bed or ankles rolling inwards.Even, Gentle Pressure and a Sense of StabilityThe splint wraps around the foot and lower leg. When the straps are adjusted properly, the pressure:Feels snug and supportive rather than tight or cutting inHelps the splint feel secure and part of the leg, not something loose or wobblySpreads contact over a wider area, reducing local pressure pointsThe pressure should never be so strong that it causes numbness, pins and needles, burning, or sharp pain. Those signs mean the straps are too tight or the angle is too strong and needs easing. Worn as intended, the splint should feel like a firm but comfortable support.Soft Padding and Breathable Materials for Night‑Long WearConsistency matters. A splint only helps if it is worn for long enough, often enough. Comfort plays a large part in whether that happens in real life.The FootReviver™ splint includes:Soft padding where it touches the shin, ankle and top of the footLightweight materials so the leg does not feel weighed downFabrics that allow air to circulate, reducing overheating and sweatingThese features are there to:Reduce rubbing over bony areasAvoid hot, stuffy discomfort that might make someone take it offMake it realistic to wear the splint for several hours at a time on most nightsBeing able to keep the splint on through much of the night increases the time that the plantar fascia and calf are held at a helpful length. This is important for changing a pattern that develops over many nights and months. If you cannot realistically sleep in a splint, it will not help, however well it is designed on paper. FootReviver™ is built so that most people can wear it for several hours without it becoming the main reason they wake up.Very soft, sock‑type splints can be comfortable but often struggle to hold the ankle and toes in a clear, consistent position. FootReviver™ combines padding with a firmer front panel, so it can maintain the angles described above while still being tolerable to sleep in.Intended Use While Sleeping and During Short RestsThe splint is mainly designed to be worn while sleeping. It can also be used during shorter rests, for example:Sitting in the evening watching televisionHaving a short nap in the afternoonIn these situations, it works in the same way: the ankle is held near a right angle and the toes are kept from dropping down, so the fascia and calf do not fully shorten between bouts of activity.It is not designed for walking or standing. The shape and lack of a sole make walking awkward and increase the risk of tripping or twisting the ankle. The splint should always be taken off before standing and only worn while sitting or lying down. The next section goes through fitting and building up use in more detail.How to Use the FootReviver™ Night SplintOnce it has been decided that a night splint is appropriate, using it properly makes a real difference. The basic aim is to fit it so the foot feels secure, the ankle sits close to a right angle, and there is a gentle, comfortable stretch rather than a strong pull.Quick fitting overviewAt a simple level, fitting the splint involves:Placing the heel fully back in the splint so the foot sits flat against the baseFastening the foot and ankle straps so the splint feels snug but not tightAdjusting the front strap or straps so the ankle sits near a right angle and the toes are just lifted enough to feel a mild stretch, not painChecking that the toes look a normal colour and feel warm, and that there is no numbness or burningThe images and step‑by‑step guide shown with this section are the best guide when you are first putting the splint on. Once you are comfortable with the basic fit, the next parts explain how to build up wear time and what sensations to expect. Adjust the angle of the Night splint to a 90 degree angle and place on your foot. Wrap the first strap around your forefoot and use the strap to properly secure it. Wrap the second strap above your ankle and secure in place using the Velcro. Fix the tension strap accordingly from your toes to the top of the night splint. Wrap the support wraps around your foot by making an X shape on the top of your foot. Make sure that the night splint is secure but not too tight!Fitting the Splint for the First TimeTo fit the splint:Sit with the leg supported and the knee slightly bent, so you can reach the straps easily.Place the foot into the splint so the heel is firmly against the back and the sole is against the base.Fasten the straps over the foot so the splint feels secure but not pinching. The toes should lie flat inside, not forced up or bent down hard.Fasten the ankle and calf straps so the splint does not wobble or slide, but also does not dig into the skin.Adjust the strap or straps that control ankle and toe position until a gentle pull is felt in the calf or under the foot. The pull should be noticeable, but not strong enough to cause sharp pain or cramp, and it should ease slightly after a few minutes.After a short time, check the toes and foot for normal warmth and colour, and make sure there is no numbness or burning. If any of these appear, loosen the straps and reduce the angle.Taking the time at the start to get a good fit helps the splint stay in the right position overnight and reduces the risk of rubbing or pressure areas.Building Up Wear Time GraduallyThe body usually needs time to get used to any new support or sustained stretch. A staged approach often works best:Begin by wearing the splint for around 1–2 hours in the evening while sitting.Once that feels comfortable, try wearing it for the first part of the night, then removing it before the final part of sleep if needed.Gradually work up, as tolerated, to wearing the splint through most or all of the night.In the early days, many people are more aware of the splint, especially when turning over. A mild pulling sensation in the calf or under the foot, and slight stiffness on removing the splint in the morning, are common and usually settle as the tissues adapt. Mild stiffness on first taking the splint off usually reflects tissues getting used to the new position rather than harm.Finding the right angle is often a matter of small adjustments over several nights rather than getting it perfect first time.If the stretch feels too strong, causes sharp pain, or disrupts sleep a lot, the angle or total wearing time is likely too much at that stage. Reducing the stretch a little and increasing use more slowly is usually a better approach than pushing through.Normal Sensations Versus Warning SignsTypical, acceptable sensations include:A gentle pull in the calf or under the foot, especially when first putting the splint onAwareness of the splint when changing position in bedA mild “just stretched” feeling on removing the splint in the morningWarning signs that need attention include:Strong, sharp pain during or after wearing the splintNumbness, ongoing pins and needles, or a “dead” feeling in the foot that does not settle quickly when the splint is taken offMarked red marks or pressure areas that do not fade within a short timeAny blisters, open areas, or broken skin under the splintIf any of these occur, stop using the splint. Either refit it very carefully with looser straps and a gentler angle or seek advice from a healthcare professional before continuing. More detailed safety information is included in the final section.Using the Splint Alongside Other Simple MeasuresThe FootReviver™ night splint usually works best when used with other simple steps that reduce strain on the plantar fascia and help it recover. This section explains how those steps link to the same pattern discussed earlier.None of these simple steps become less important because you use a night splint; if anything, they work best together.Adjusting Activities That Clearly Aggravate SymptomsActivities that clearly make pain worse, such as:Long spells of standing on very hard floors without a breakSudden jumps in walking or running distanceHigh‑impact exercise on already painful heelsadd to the total stress the plantar fascia has to handle. When this keeps happening, the sore patch near the heel can stay irritated.Adjusting activities might mean:Breaking up long periods of standing with short spells of sitting if possibleBuilding up walking or running distance gradually rather than in leapsTemporarily reducing or altering impact exercise while pain is severeThese changes reduce how often and how strongly the fascia is stressed during the day. Together with the splint’s effect on what happens between bouts of activity, this helps reduce both day‑time and first‑step strain.Stretching and Keeping the Calf and Plantar Fascia MobileGentle stretches can help ease general tightness around the heel. Examples include:Calf stretches against a wall or off a stepPlantar fascia stretches, such as sitting and gently drawing the toes up towards the shinThese work on the same tissues that the night splint holds in a longer position overnight. Stretching helps those tissues move more freely during the day. The splint then helps stop them shortening fully again when off the feet. Both aim to reduce the size of the jump in length when standing and walking.Building Strength in the Foot and CalfStronger muscles in the foot and calf help:Share forces more evenlySupport the arch and ankle betterMake the whole system more tolerant of daily demandsProgressive strengthening means starting with easier exercises and gradually increasing the effort. For example:Begin with simple heel raises on flat ground, gently lifting and loweringLater, progress to lifting up and slowly lowering down from a stepIncrease repetitions as comfort allows, guided by symptoms and, ideally, by a physiotherapistImproving strength and control means less strain ends up going through the sore spot near the heel with each step. Combined with a night splint that reduces sudden strain after rests, this can help shift the plantar fascia towards a more robust, less easily provoked state.Supportive Footwear and, Where Needed, InsolesShoes make a big difference to how much force travels through the heel and arch. Helpful features include:Decent cushioning under the heel to soften impact on hard surfacesA supportive heel cup to help hold the heel steadyA sole that is reasonably firm and not overly floppy or twistingThin, very flat, or very worn‑out shoes often have little cushioning or support, so more shock and strain go straight through the plantar fascia.In some cases, arch support insoles can help, especially where the foot rolls in a lot or the arches are high and rigid. By helping to hold the arch at a more supported height, these can reduce how much the fascia is stretched and strained during the day.Supportive shoes and insoles help control how much the plantar fascia is stressed with each step during the day, while the night splint helps stop the fascia and calf shortening back fully between those periods on your feet. Used together, they help smooth out the peaks of load on the plantar fascia.When Physiotherapy or Podiatry Input HelpsSeeing a physiotherapist or podiatrist is particularly helpful when:Pain has been present for many monthsThere is uncertainty about the diagnosisThere are other joint or tendon problems as wellBasic self‑care has not made enough differenceA clinician can:Assess how the foot, ankle, and leg moveIdentify particular weaknesses or stiff areasPrescribe tailored exercisesAdvise on footwear, insoles, and activity levelsIn that setting, a night splint is one part of the plan. It deals with what happens when the foot is off the ground and resting, while exercises and footwear changes deal with what happens when standing and walking.Left to grind on, this pattern often leads people to quietly change how they walk, which can start to upset other parts of the foot, ankle, knee or hip. Addressing it properly, with day and night measures working together, makes this less likely.What to Expect Over TimeIf the splint suits your pattern of pain and is used regularly alongside the daytime steps described above, this is how symptoms often change over time. Responses vary, but there are common patterns. It helps to separate getting used to the splint from changes in pain, and to have realistic expectations about timing.Getting Used to Wearing the SplintIn the first week or two, the main changes are about comfort and awareness, such as:Noticing the splint more when settling to sleep or turning overFeeling a mild pull in the calf or under the foot when first putting it onA slight “just stretched” feeling when taking it off in the morningThese usually settle as you find a comfortable angle and strap tension and as the tissues adapt to being held in a slightly different position. This stage is more about adjustment than about big changes in pain.Early Changes You May NoticeOver the next 2–4 weeks, once you are used to wearing the splint for longer periods, many people notice:The first steps in the morning are still noticeable but less sharply painfulThe time spent hobbling at the start of the day reducesStanding after sitting or driving produces less of a jolt through the heelThese changes reflect the pattern described earlier: because the fascia and calf are no longer allowed to shorten fully when resting, each restart involves a smaller, slower stretch through the sore area. That tends to be easier for irritated tissue to cope with. This is often when the benefit of taking the sharp edge off those first few steps becomes most obvious.Longer‑Term Changes and Clear LimitsWith steady night‑time use and good daytime choices, clearer improvements in morning and “after rest” pain are often reported over 4–6 weeks and beyond. For some people, this may mean:Waking up without dreading the first few stepsBeing able to walk more freely first thingHaving more confidence to be on their feet at work or in daily lifeIt is important to stay realistic:A night splint helps many people, but not everyone responds in the same way.In some, pain is driven by other structures or conditions that need different treatment.If pain does not change, or becomes worse, despite a fair trial of regular use and sensible daytime measures, a further assessment is needed to confirm what is going on and plan next steps.If you notice a clear, consistent improvement in how your first steps feel, it usually makes sense to keep using the splint and the other measures for long enough to make that improvement more stable, rather than stopping as soon as things ease. For many people, improvements follow this kind of pattern, but it is not the same for everyone. Some may notice changes sooner, others later, and some may need different or additional treatments.Factors That Influence How Well It HelpsHow quickly and how much things improve depends on several factors, including:How long the problem has been present and how severe it isBodyweight and general healthJob and daily activity levels, especially standing on hard floorsHow the foot is shaped and how it movesHow consistently the splint is used and how well the angle is adjustedWhether supportive shoes, insoles, and exercises are also in placeThese help explain why two people with seemingly similar pain can respond quite differently to the same support.If, after a fair trial using it as directed, you notice no meaningful change in how your first steps feel, it is reasonable to stop and seek further assessment rather than persisting out of hope alone.Who This Night Splint Is and Is Not Suitable ForThis section is a quick guide to who is likely to benefit from a night splint of this type and when it is important to speak to a clinician before using one.People Likely to BenefitThe FootReviver™ night splint is particularly aimed at the pattern described earlier, where:Heel or arch pain is most noticeable with the first steps after sleepSimilar “start‑up” pain appears when standing after sitting or drivingThere is a diagnosis or strong suspicion of plantar fasciitis or plantar heel painPersistent morning pain remains despite trying simple measures such as stretching and supportive footwearIt may also have a role, under professional advice, in some Achilles tendon problems and certain ankle stability issues where overnight posture and tissue length clearly affect symptoms.When to Speak to a Clinician Before Using ItSpeak to a GP, physiotherapist or podiatrist before using this splint if any of the following apply:Diabetes, especially with:A history of foot ulcersReduced feeling in the feet (neuropathy)Known poor circulation to the legs or feetKnown circulation problems in the legs or feet, such as peripheral arterial disease or previous vascular surgeryNerve‑related problems in the legs or feet that cause major weakness, loss of feeling, or altered position senseSkin issues in the area the splint would cover, including:UlcersOpen woundsVery fragile or easily damaged skinRecent surgery or major injury to the foot, ankle, or lower leg, unless a surgeon or clinician has specifically recommended a night splintVery stiff ankles or fixed deformity, where the foot cannot be comfortably brought near a right angleIn these situations, strap pressure and changes in joint position need careful consideration, as changes in feeling, blood flow, or skin strength can make pressure‑related damage more likely.When a Splint Is Not the Right First StepDo not rely on a night splint as the first or only response when there are signs that something more serious or different may be present. Instead, seek medical advice if:Pain starts suddenly and severely, particularly after a fall, twist, or impactThe heel or ankle is very red, hot, or swollenPain is present at night and does not ease with restThere are general symptoms such as fever, unexplained weight loss, or feeling generally unwellThere is unexplained numbness, burning, or tingling in the foot or toesPain is spreading, or affecting both feet in an unusual or worrying wayThere is a known history of inflammatory arthritis, autoimmune disease, or other systemic illnessThese features can point to conditions such as stress fractures, inflammatory joint problems, or nerve issues that need proper assessment and treatment.More detailed safety information and advice are included in the final section.Other Conditions This Night Splint Can Help SupportThe FootReviver™ night splint is designed first and foremost for plantar fasciitis and related heel pain. However, because it positions the ankle and foot in a set way, it can also play a part in managing some other problems where overnight posture and tissue length matter.In these situations, it is usually one element in the overall plan, not the only measure. It is often best to use it on the advice of a clinician who understands your specific condition.If your main issue is classic plantar fasciitis with morning and after‑rest heel pain, you may wish to move on to the next section. If you have been told you have one of the conditions below, the detailed overviews may help explain where a night splint could fit.Achilles tendon pain and stiffnessOverviewPain and stiffness at the back of the heel or lower leg, especially with the first few steps in the morning, are often linked to problems in the Achilles tendon. Many people also notice pain when going downstairs, walking up or down slopes, or starting a run. Things may ease as the tendon warms up, only to ache again later if activity has been heavy.This pattern is common in people who run or walk a lot, play running‑based sports, or have jobs that keep them on their feet for long periods. It can also begin after a sudden increase in activity, such as starting a new exercise routine or taking on a more active role at work.What is happening in the Achilles tendonThe Achilles tendon connects the calf muscles to the back of the heel bone. It has to cope with the forces of walking, running, climbing stairs, and pushing off the ground. When it is repeatedly asked to do more than it can comfortably handle, without enough recovery, small areas within the tendon can begin to show wear and irritation. This is often called an irritable tendon (tendinopathy).Over time, the tendon can:Become thicker and less spring‑like in certain spotsBecome more sensitive to being stretched or loadedRecover more slowly between periods of useBecause the tendon attaches just above the heel bone, any time the ankle bends up (such as when taking a step, going downstairs, or running), that sore area is asked to lengthen and take load.How Achilles pain behaves during movementAchilles problems often follow a recognisable pattern. Common features include:Stiffness and pain with the first steps in the morningDiscomfort when walking downstairs or down slopesPain at the start of a run or brisk walk that eases as the tendon warms upA return of aching later in the day or after a harder sessionThis is because an irritable tendon struggles with sudden or high‑demand stretching and loading. When it is cold and slightly shortened, those first movements ask a lot of it. Once the tendon has warmed and adjusted to the load, it often feels better, but if the total load is still more than it can handle, it tends to ache again later.What rest and sleep do to the AchillesWhen off the feet, the calf muscles and Achilles tendon naturally shorten a little. At night, common sleep positions can increase this:Toes pointing down when lying on the backFeet hanging over the edge of the mattress so the ankle is pulled into a more pointed positionOne leg resting over the other, twisting the ankle inwards or outwardsFor someone with an irritable Achilles tendon, these positions let the calf–Achilles complex shorten more and stay short for hours. By morning, the tendon is often stiffer and less ready to move.When then:Standing up and walking on a flat floorGoing downstairs straight awaySetting off for a walk or runthe tendon is suddenly asked to lengthen and take weight at the same time. That combination produces the classic morning stiffness and pain. As with plantar fasciitis, much of this morning discomfort comes from tissues that have shortened overnight and are then forced to move and bear weight in one go.How the FootReviver™ night splint can help Achilles painThe FootReviver™ night splint holds the ankle closer to a right angle and gently lifts the toes towards the shin. This position keeps the calf muscles and Achilles tendon nearer to their daytime length instead of letting them shorten fully.That can:Reduce how far the tendon has to lengthen with the first few stepsMake those first movements less abrupt and less painfulLimit extreme toes‑down positions that can aggravate the tendon overnightBy keeping the tendon at a more neutral length overnight, the splint helps cut down the shock it feels each time you start moving again in the morning or after sitting. It also supports the gains from a sensible strengthening and loading programme, rather than allowing the tendon to tighten back fully each night.How it fits alongside Achilles rehabilitationFor Achilles tendinopathy, a well‑planned strengthening and loading programme and sensible changes in activity are usually central to recovery. This often includes:Gradual calf strengthening exercises, often with controlled lowering of the heel from a raised position, as prescribed by a physiotherapistAdjusting running or walking distances and speeds to a level the tendon can tolerateReviewing footwear, including heel height and cushioning, to avoid sudden changes the tendon cannot cope withA night splint does not replace any of this. Its main job is to reduce the extra strain created by starting each day, or each walk after a rest, with a stiff, shortened tendon. That can mean less morning stiffness, a smoother start to exercise, and better tolerance for day‑to‑day activities.When to seek assessment before using a night splint for Achilles problemsIt is important to have the tendon properly checked before relying on a splint alone if:Pain came on suddenly with a feeling of a snap or popThere is marked swelling or a visible gap in the tendonYou cannot push off properly or stand on tiptoe on that legPain is severe at the point where the tendon joins the heel bone (insertional pain)Sudden severe symptoms can suggest a partial or complete tear, or other conditions that need specific management. In insertional problems, too much stretch can sometimes aggravate the issue, so angle settings need to be cautious and guided by a clinician. Even in gradual‑onset Achilles pain, a physiotherapist or podiatrist can help design a suitable exercise and load plan, with the night splint used as one supportive element.Inner ankle tendon problems and ankle instabilityOverviewPain and a tired, aching feeling on the inside of the ankle and under the arch, with a sense that the foot is “rolling in” or the ankle is less steady, are common complaints. People may notice swelling around the inner ankle bone, aching in the arch after standing, and the impression that one foot looks flatter than it used to.These are often signs that the structures supporting the inner side of the ankle and arch are under strain. The main tendon here is the posterior tibial tendon, supported by ligaments that help hold the bones of the foot and ankle in a good position.What the inner ankle tendon and ligaments doThe posterior tibial tendon:Runs behind the inner ankle boneFans out under the arch of the footHelps support the arch and control how much the foot rolls inwards when walkingLigaments along and under the inner ankle work with this tendon to:Stop the arch collapsing too farLimit how far the ankle rolls inwardsHelp the foot act as a firm, controlled base when standing and walkingWhen these tissues are working well, the inner ankle and arch can cope with everyday loads without pain.How strain and gradual change can build upInner ankle tendon and ligament problems often develop slowly rather than from a single event. Common patterns include:Long hours standing or walking on flat, hard floors that give little natural cushioningRegular use of flat, unsupportive shoesExtra bodyweight increasing load through the inner footA natural tendency towards flatter feet or more inward rollIn these situations, the posterior tibial tendon and inner ligaments have to work harder to hold the arch up and control movement. Over time they can become strained and weaker, and the arch can begin to sit lower.People may then notice:Aching or sharp pain along the inside of the ankle and under the archSwelling around the inner ankleThe foot looking flatter or rolled in compared to the other sideA sense that the ankle is less steady, especially on uneven groundWhat rest and sleep positions can do to the inner ankleDuring the day, if the arch is collapsing inwards or the ankle is rolling in often, the inner ankle structures are constantly being pulled. Rest can give some relief, but the way the foot rests overnight also plays a role.Typical sleep positions can:Leave one foot resting with the top of the other foot pressing across it, twisting the ankleAllow the ankle to roll inwards so that the inner side is held under tension for long periodsLet the arch “hang” in a flattened position without supportFor an already strained tendon or ligament, being held all night in a rolled‑in or twisted position can mean:Waking up with a very tired, achy inner ankleFeeling as if the arch has “collapsed” again as soon as you standA sense of instability even before much walking has been doneAs described earlier, hard, flat floors pass more force straight through the foot. For inner ankle problems this means even more work for the tendon and ligaments, making it especially helpful if night‑time positions do not add extra strain.How the FootReviver™ night splint can support inner ankle problemsThe FootReviver™ night splint holds the ankle closer to a neutral position while you sleep. This means:The heel and lower leg are kept more in line, with less inward or outward rollThe arch is less likely to be held in an extreme collapsed posture overnightTwisting positions, where one foot lies heavily over the other, are harder to fall intoFor the posterior tibial tendon and inner ankle ligaments, this can:Reduce repeated overnight pulling on tired tissuesHelp the arch and ankle feel less “collapsed” or drained when first getting upProvide a calmer period for strained structures to settle between days on the feetThe splint does not push the arch up on its own, but by helping to keep the ankle and heel steadier at rest, it may reduce the extra strain these tissues face. Where footwear and insoles support the arch and ankle during the day, the night splint helps stop the ankle drifting into positions at night that undo that support.Why daytime support is especially important hereFor inner ankle problems and arch collapse, daytime alignment and support are often the main drivers of change. Helpful steps usually include:Wearing shoes with a firm, supportive heel cup and a stable soleUsing arch‑support insoles or ankle braces where advised by a clinicianStrengthening the muscles that support the arch and control ankle movementReducing or breaking up long periods of unsupported standing on hard floors where possibleIn this setting, the FootReviver™ night splint can be a useful add‑on. It aims to stop night‑time positions from undoing the support and strengthening work done during the day.Limits and when to seek further assessmentA night splint cannot reverse marked flattening of the foot or severe posterior tibial tendon problems on its own. It should not be seen as a substitute for:A proper assessment of foot shape, joint condition, and tendon healthThe right combination of footwear, insoles and, in some cases, ankle bracingTargeted strengthening, stretching, and activity guidanceIt is especially important to seek specialist advice if:The arch appears to be flattening more over timeThe ankle feels very unstable or there are frequent sprainsPain is severe, or walking even short distances is difficultIn such cases, a foot and ankle specialist or experienced physiotherapist can decide whether a night splint has a role as part of a more detailed plan.Nerve-related foot and ankle conditionsOverviewSome foot and ankle problems are mainly driven by how nerves and muscles are working, rather than by the plantar fascia or the main tendons alone. These can include:Conditions where a nerve around the ankle is being irritated or compressedSituations where weakness or changes in muscle balance affect how the foot sits and movesThese problems are more complex than straightforward plantar fasciitis or tendon issues, and decisions about supports such as night splints are best made with help from a clinician. This overview explains, in general terms, where a splint like the FootReviver™ may fit in, and why professional guidance is important.Nerve compression around the ankleOn the inside of the ankle there is a narrow space through which tendons, blood vessels, and a nerve pass towards the foot. If structures in this area become swollen or the space becomes tighter, the nerve can be squeezed. This is often referred to as a tarsal tunnel‑type problem.Typical features include:Burning, tingling, or numbness in the sole of the foot or toesPain or discomfort along the inside of the ankle, sometimes worse at nightSymptoms that may be aggravated by long standing or certain foot positionsThe way the ankle is positioned can influence how much pressure is placed on this nerve. Rolling the ankle inwards for long periods, or holding it twisted, may narrow spaces and increase irritation.Weakness and altered control: foot drop and neuromuscular conditionsIn some conditions, nerves and muscles are weakened or their control is altered. Examples include:Mild foot drop, where lifting the front of the foot is difficult because the muscles on the front of the shin are weakCertain inherited nerve or muscle conditions, such as Charcot‑Marie‑Tooth disease, which can cause:High archesClawed toesChanges in how the foot rests and movesIn these situations:The foot may tend to sit in a pointed‑down position, especially when relaxed or lying downSome muscles overpower others, pulling the foot into awkward positionsThere is a risk that joints around the ankle and foot become stiff and lose movement (contractures), making walking and putting footwear on more difficult over timeIn some people, nerve‑related weakness or compression exists alongside plantar fasciitis or Achilles problems, so symptoms and patterns can overlap.How night‑time position can affect nerve‑related conditionsFor nerve compression problems:Sleeping positions that roll the ankle inwards or twist it sharply can keep pressure on the nerve for hours at a timeThis can contribute to night‑time tingling, burning, or painFor weakness or neuromuscular conditions:Allowing the ankle to drop into a very pointed position all night encourages calf muscles and the Achilles tendon to shortenStructures at the front of the ankle can become tightOver time, it may become harder to bring the foot up towards a right angle, affecting walking and balanceIn both groups, how the foot and ankle are held, and for how long, can make a meaningful difference to symptoms and joint movement.Where a night splint might play a roleBecause the FootReviver™ night splint holds the ankle nearer to a right angle and limits twisting, it can sometimes play a part in managing certain nerve‑related issues, always under proper guidance.Possible roles include:For some tarsal tunnel‑type problems:Keeping the ankle closer to neutral, rather than rolled inwards, may reduce how much pressure is placed on the nerve during sleepLimiting extreme inward twist may help with night‑time symptom control in selected casesFor mild foot drop or some neuromuscular conditions:Holding the ankle near a right angle and the toes slightly up can:Reduce time spent in a fully pointed, “dropped” positionHelp slow the development of tightness in the calf and front of the ankleMaintain more useful movement at the ankle for walking and transfersThese uses are more specialised than the typical plantar fasciitis pattern. The aim here is often to help maintain range and reduce aggravation, rather than to remove the underlying problem.Why professional supervision is essentialNerve‑related problems vary greatly between individuals. What is helpful for one person could be unhelpful or unsafe for another. Important reasons for involving a clinician include:Altered sensation:Reduced feeling in the foot can mean pressure from straps or padding is not noticed early, increasing the risk of skin damageCirculation changes:Some neuromuscular conditions carry a higher risk of circulation issues, which can affect how much pressure and stretch are safeVarying joint positions:Fixed deformities or marked stiffness may make certain angles uncomfortable or unsafeDoctors, neurologists, rehabilitation specialists, physiotherapists, or podiatrists can:Confirm the diagnosis and main drivers of symptomsDecide whether a night splint is appropriate, and if so, how it should be set upAdvise on a safe angle and wearing timeCheck for unwanted changes in skin, sensation, or symptoms over timeIf a clinician does recommend using a night splint, it is especially important to monitor any increase in burning, tingling, numbness, or new pain and to report these promptly.Who should avoid using a night splint without specialist adviceA night splint should not be used without direct guidance in people who:Have very limited or absent feeling in their feetHave severe deformity or fixed joint positions at the ankle or midfootAre noticing rapidly changing weakness or new nerve symptomsHave active ulcers, open wounds, or very fragile skin where the splint would sitIn these situations, the risks from pressure, restricted blood flow, or incorrect positioning are higher, and specialist care is required.For people with milder nerve‑related problems, and with clear advice from a clinician, a night splint like FootReviver™ can sometimes form one part of a wider plan. Its role in that context is to help control how the foot and ankle rest overnight, support safer joint positions, and reduce some of the extra strain that certain postures place on sensitive nerves and weakened muscles.Why Choose the FootReviver™ Night Splint from NuovahealthThe FootReviver™ Plantar Fasciitis Night Splint has been put together around the patterns commonly seen in people with heel and Achilles pain:Pain that is especially bad with the first steps after restCalf muscles and plantar fascia that tighten when the foot is off the groundA need for something that can realistically be worn at night, not just in theoryKey points about this particular splint include:It holds the ankle and toes in a controlled, gently stretched position that targets both the plantar fascia under the heel and the calf–Achilles at the back of the ankle, without forcing the foot into an extreme or rigid angle.It is built for night‑time use, with padding, breathable fabrics, and adjustable straps, so most people can wear it for several hours without excessive discomfort.The adjustable design allows people to start with a milder stretch and then increase it over time, which is often important in long‑standing or very sensitive pain.The way it sets the foot and ankle can also help support some related tendon and ankle alignment problems, when used under professional guidance.The strap positions, padding and angle range have been adjusted based on where clinicians regularly see people develop rubbing, pressure and discomfort — across the front of the ankle, the shin and the top of the foot — so the splint reflects how these conditions behave in day‑to‑day life, not just in theory.There is a 30‑day money‑back guarantee, so it can be tried as directed for a reasonable period. The guarantee is there so you can give it a fair trial, wearing it as directed. If, after that period, it has not helped in the way hoped, it can be returned.Because the position it holds is central to several common problems — plantar fasciitis, Achilles pain, and some inner‑ankle issues — it was designed from the outset to support not only classic plantar fasciitis, but also the Achilles and inner‑ankle patterns clinicians see again and again, when used under appropriate guidance. Many basic night splints hold the ankle in one fixed position. FootReviver™ is built to be more forgiving and adjustable, recognising that sore, long‑standing tissue rarely tolerates a “one‑size‑fits‑all” angle from day one.Making Mornings Easier AgainBy this point, the picture should be clearer: much of that first‑step pain comes from the way sore tissues behave when you are off your feet, not just from what you do when you are on them. Getting out of bed, walking to the bathroom, or standing up after sitting for a while can turn into something to brace for instead of something hardly noticed.In simple terms, the pattern involves:A sore patch in the plantar fascia near the heel, often from repeated overloadCalf and Achilles tissues that naturally shorten when the foot is off the groundCommon sleeping and resting positions that let these tissues shorten fullyFirst steps after rest that pull on them sharply with bodyweightThe FootReviver™ Plantar Fasciitis Night Splint is designed to change what happens during those resting periods. By holding the ankle near a right angle and gently lifting the toes, it keeps the plantar fascia and calf closer to their working length overnight and during rests. That reduces the sudden pull on sore tissue when standing and helps those first steps feel less like a shock.For many people whose pain follows this pattern, using a night splint steadily, alongside sensible daytime measures, can mean:Less dread about getting out of bedFewer painful, shuffling steps first thingGreater confidence about walking and standing at work and at homeIf your heel or arch pain is at its worst with the first steps after sleep or sitting, and none of the safety cautions apply, the FootReviver™ night splint is a sensible, mechanism‑based option to consider trying for a few weeks. Wearing it most nights and combining it with the daytime steps outlined above gives it a fair chance to take the sharp edge off those first few steps after sleep and sitting.It is not a guaranteed cure, but it is a realistic way to tackle one of the key mechanical drivers of plantar fasciitis‑type pain while you rest, rather than simply masking symptoms. The details here are general; a GP, physiotherapist or podiatrist can advise how this fits with your own situation.Important Information and Health DisclaimerThe information on this page is general and is not a substitute for an assessment or advice from a GP, physiotherapist, podiatrist, or other qualified clinician. It is written for adult readers in the UK. No specific outcome can be guaranteed and responses vary from person to person.When to Get Advice Before Using This ProductThe FootReviver™ Plantar Fasciitis Night Splint is designed as a support for common soft‑tissue problems around the heel and ankle, especially plantar fasciitis and some tendon issues. It does not replace a proper medical assessment, diagnosis, or full treatment plan.Speak to a GP, physiotherapist, podiatrist or other suitable clinician before using this product if you have:Diabetes, particularly if there is a history of:Foot ulcersReduced feeling in the feet (neuropathy)Poor circulation in the legs or feetCirculation problems, such as:Known peripheral arterial diseasePrevious vascular surgery or known poor blood flow to the legsNerve‑related conditions affecting the legs or feet that cause major weakness or loss of feelingSkin problems in the area the splint would cover, including:UlcersOpen woundsVery fragile or thin skin that breaks easilyRecent surgery or major injury to the foot, ankle, or lower leg, unless a surgeon or clinician has specifically advised that this kind of splint is appropriateMarked swelling, redness, warmth, or obvious deformity of the heel, ankle, or footA history of blood clots in the legs (deep vein thrombosis) or known clotting disordersVery stiff ankles or fixed deformity, where the foot cannot be comfortably brought close to a right angleBecause the splint uses straps and gentle pressure to hold the foot in position, people with circulation, nerve, or skin problems may be at greater risk of pressure‑related damage if it is used inappropriately. Professional advice helps balance these risks against any potential benefit.Serious Symptoms That Need Prompt Medical AssessmentA night splint can reduce pain, especially the sharp pain on first standing. Less pain does not always mean the underlying cause has been fully dealt with. Do not rely on a splint alone if:Pain starts suddenly and severely, particularly after an injury, fall, or impactThe heel or ankle is very red, hot, or swollenPain is present at night and does not ease with restThere are general symptoms such as fever, unexplained weight loss, or feeling generally unwellThere is unexplained numbness, burning, or tingling in the foot or toesPain is spreading, or affecting both feet in an unusual or worrying wayThere is a history of inflammatory arthritis, autoimmune disease, or other systemic illnessThese signs can point to problems such as stress fractures, inflammatory joint disease, or nerve conditions that need proper medical assessment and treatment.Not a Stand‑Alone Cure for Plantar FasciitisThe FootReviver™ night splint is intended to be part of sensible care for plantar fasciitis and related problems, not the only step taken.Using a splint without also:Adjusting clearly aggravating activities where possibleReviewing footwear and using insoles if neededWorking on stretching and strengtheningSeeking help if pain is not improvingcan leave the underlying problem unaddressed. If plantar fasciitis is left to rumble on or only partly treated, pain can become long‑term. Many people then change the way they stand and walk to avoid loading the sore area. Over time, this can put extra strain on:Other parts of the footThe ankle and Achilles tendonThe knees, hips, and lower backThese knock‑on effects are another reason to deal with plantar fasciitis properly, rather than just taking the edge off the pain.When to Stop Using the Splint and Seek Further AdviceStop using the splint and get advice promptly if:The foot becomes very cold, very pale, or develops unusual colour changes while the splint is onNumbness, ongoing pins and needles, or a “dead” feeling develops in the foot and does not settle quickly after taking the splint offThere are blisters, open areas, or broken skin under any part of the splintPain under or around the splint is severe or clearly worseningThese signs suggest that the splint may be too tight, poorly fitted, or not right for your situation.If in Doubt, Get It CheckedThe FootReviver™ Plantar Fasciitis Night Splint is a carefully thought‑through support for common patterns of heel and tendon pain, but it will not suit everyone or every cause of heel pain. If there is any doubt about whether it is appropriate, or if symptoms are not improving as hoped, it is always sensible to arrange to speak to a GP, physiotherapist or podiatrist for assessment and tailored advice, rather than trying to manage the problem alone.
Foot Supports